How to Restore Gut Flora-Test, After Antibiotics, Foods & Supplements
With digestive disorders and microbiome issues taking the headlines left and right, many of us are wondering just how healthy our guts are. That is why improving or restoring your gut flora is crucial. After all, the state of your gut can influence your immune function, risk of chronic disease, allergies, autoimmune reactions, food intolerances, and possibly even our body weight among countless other things. In this article, find out ways to test the health of gut flora and how to restore in.
What is Gut Flora Imbalance
Gut Flora
It is the complex community of microorganisms that live in the digestive tracts of humans and other animals, including insects. The gut metagenome is the aggregate of all the genomes of gut microbiota.
Intestinal flora: harmless microorganisms that inhabit the intestinal tract and are essential for its normal functioning.
Gut Flora Imbalance
This is when there is no balance of normal bacterial flora. It is when the amount of bad gut bacteria is too much. It is referred to as dysbacteriosis. Here are some of the signs the problem affects you.
Below are some of the Symtoms and Signs of Gut Flora Imbalance
- Constipation
- Excess intestinal gas
- Too little or no intestinal gas
- Chronic diarrhea
- Hormonal problems
- PMS
- Menstrual complaints
- Prostate trouble
- Breast enlargement in men
- Need for sexual hormone medication
- Candidainfection (candidiasis)
- Chronic anemia
- Chronic respiratory problems
Checking your Gut Flora- Gut Health Tests you can do at Home
Number of professional tests can help diagnose leaky gut; SIBO and other forms of gut dysbiosis; infections like C. difficile and H. pylori; parasite infection; inefficient digestion of fats, proteins and/or carbohydrates; and of course, diseases of the gut like diverticular disease, ulcerative colitis, and celiac disease. Certainly, if you are worried about a serious health issue, it’s imperative to go to your doctor and have a detailed conversation. Fortunately, there are a few tests you can do at home to gauge the state of your gut health and see if you have indications of a problem.
These are some of the test that you can do at home;
Transit Time Test
A bowel transit time test measures how long it takes for food to travel through the digestive tract. As eat your food it moves into your stomach, where it is mixed with acid and digestive enzymes.it then leaves the stomach and then squeezed through your small intestine, where nutrients are absorbed for use by your body. The food then goes into your large intestine where water is absorbed. Whatever hasn’t been digested and absorbed by your intestines combines with bacteria and other waste products and becomes stool .Stool is expelled from your body through your anus.
The time it takes for food to travel from your mouth through your digestive tract to your anus is your bowel transit time. Sometimes, just the time it takes for food to travel through the colon is measured. This is called the colonic transit time.
Bowel transit time depends on what types of food you eat and how much you drink. For example, people who eat lots of fruits, vegetables, and whole grains tend to have shorter transit times than people who eat mostly sugars and starches. Because different people have different transit times, experts disagree about how useful this test is.
For this test, you swallow one or more gel capsules filled with markers that will show up on an X-ray. The markers look like white spots A or rings in the X-ray pictures. When you will have X-rays depends on the type of test done. Most commonly, you will have an X-ray test 5 days after swallowing the markers. This will show how the markers have moved through your intestines or you may swallow multiple capsules full of markers on three days in a row. In this case, you will have X-ray tests on multiple days to check the progress of the markers through your intestines.
Many of the following foods will do the trick:
- Sesame seeds
- Corn kernels
- Red beets
How it works
whichever food is used, you simply note the time you eat it, and then watch and wait for then it re-appears in a bowel movement. Sesame seeds or corn will be easy to spot, and beets will give a distinct purple-red color. Keep in mind, beets can pigment urine as well, so don’t get worried if you see some pinkish pee.
In optimal transit time is considered to be 12 to 48 ours. Longer than 72 hours indicates constipation and he possibility of other gut pathologies.
Bristol Stool Form Scale
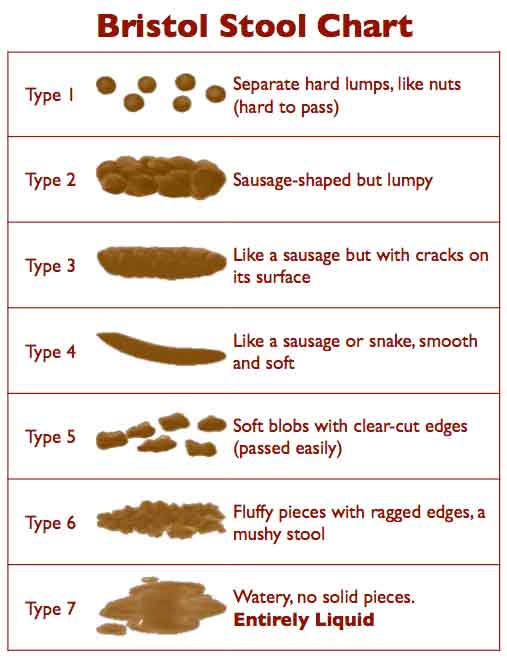
The Bristol stool scale, Bristol stool chart (BSC), Bristol stool form scale, or BSF scale is a visual aid that classifies faeces into seven different categories, and was first developed in the 1990s by researchers at the university of Bristol (hence the name!) to help distinguish abnormal bowel movements from healthy ones. Here are the categories and description, courtesy of Gutsense.org.
Type 1: Separate hard lumps, like nuts
Typical for acute dysbacteriosis. These stools lack a normal amorphous quality, because bacteria are missing and there is nothing to retain water.
The lumps are hard and abrasive, the typical diameter ranges from 1 to 2 cm, and they‘re painful to pass, because the lumps are hard and scratchy.
There is a high likelihood of anorectal bleeding from mechanical laceration of the anal canal. Typical for post-antibiotic treatments and for people attempting fiber-free diets. Flatulence isn‘t likely, because fermentation of fiber isn‘t taking place.
Type 2: Sausage-like but lumpy
Represents a combination of Type 1 stools impacted into a single mass and lumped together by fiber components and some bacteria. Typical for organic constipation. The diameter is 3 to 4 cm.
This type is the most destructive by far because its size is near or exceeds the maximum opening of the anal canal‘s aperture (3.5 cm). It is bound to cause extreme straining during elimination, and most likely to cause anal canal laceration, hemorrhoidal prolapse, or diverticulosis.
To attain this form, the stools must be in the colon for at least several weeks instead of the normal 72 hours. Anorectal pain, hemorrhoidal disease, anal fissures, withholding or delaying of defecation, and a history of chronic constipation are the most likely causes. Minor flatulence is probable.
A person experiencing these stools is most likely to suffer from irritable bowel syndrome because of continuous pressure of large stools on the intestinal walls. The possibility of obstruction of the small intestine is high, because the large intestine is filled to capacity with stools.
Adding supplemental fiber to expel these stools is dangerous, because the expanded fiber has no place to go, and may cause hernia, obstruction, or perforation of the small and large intestine alike.
Type 3: Like a sausage but with cracks in the surface
This form has all of the characteristics of Type 2 stools, but the transit time is faster, between one and two weeks. Typical for latent constipation. The diameter is 2 to 3.5 cm. Irritable bowel syndrome is likely.
Flatulence is minor, because of dysbacteriosis. The fact that it hasn‘t become as enlarged as Type 2 suggests that the defecations are regular. Straining is required. All of the adverse effects typical for Type 2 stools are likely for type 3, especially the rapid deterioration of hemorrhoidal disease.
Type 4: Like a sausage or snake, smooth and soft
This form is normal for someone defecating once daily. The diameter is 1 to 2 cm. The larger diameter suggests a longer transit time or a large amount of dietary fiber in the diet.
Type 5: Soft blobs with clear-cut edges
It is typical for a person who has stools twice or three times daily, after major meals.
Type 6: Fluffy pieces with ragged edges, a mushy stool
This form is close to the margins of comfort in several respects.
First, it may be difficult to control the urge, especially when you don‘t have immediate access to a bathroom.
Second, it is a rather messy affair to manage with toilet paper alone, unless you have access to a flexible shower or bidet. Otherwise, consider it borderline normal.
These kinds of stools may suggest a slightly hyperactive colon, excess dietary potassium, or sudden dehydration or spike in blood pressure related to stress.
It can also indicate a hypersensitive personality prone to stress, too many spices, drinking water with a high mineral content, or the use of mineral salts.
Type 7: Watery, no solid pieces
This, of course, is diarrhea, a subject outside the scope of this chapter with just one important and notable exception—so-called paradoxical diarrhea. It‘s typical for people affected by fecal impaction—a condition that follows or accompanies type 1 stools.
During paradoxical diarrhea the liquid contents of the small intestine have no place to go but down, because the large intestine is stuffed with impacted stools throughout its entire length. Some water gets absorbed; the rest accumulates in the rectum.
The reason this type of diarrhea is called paradoxical is not because its nature isn‘t known or understood, but because being severely constipated and experiencing diarrhea all at once, is, indeed, a paradoxical situation. Sourced from Gutsence.org
Visual Inspection
Some other visual indicators can tell you a lot about your gut health.
Some are;
Floating poop:
stools that float to the surface in the toilet are usually caused by diet-induced gas, but they can also result from a bowel infection, lactose intolerance, pancreatic diseases, gallbladder diseases, and certain other health conditions.
If no other symptoms are present, floaters usually don’t indicate a problem. But, when accompanied by gastrointestinal distress or other signs of gut dysbiosis, or when extremely consistent, they might point to an underlying disorder, or a gut microbe imbalance.
Indigested food particles
When you can spot obvious food particles in our stools, there can be a few different causes, some of them harmless, others that indicate a potential problem. Not chewing well enough, gulping large amounts of liquid while eating, eating too quickly, and consuming hard-to-digest foods like small seeds, nuts, corn can all lead to unwanted food particle sightings.
Bowel Movement Frequency
Bowel movement frequency can tell you about the state of your gut health. Although there aren’t a specific, ideal number of bowel movements each person should have every day.A frequency of three times per day to three times per week is generally considered fine.
If you do find yourself on the lower end of the normal pectrum, it may indicate that it’s time to up your vegetable intake.
Gut Flora Specialist Testing
The gastrointestinal tract has two main functions;
- To digest and absorb important nutrients for the body’s growth and function
- To act as a barrier to keep harmful substances and microorganisms from entering the blood.
Within the gastrointestinal tract thousands of different bacterial species can be found. These bacteria also play a key role in digestion, nutrition, pathogen defence and immune system development.
When the function and interplay within this complex system is disturbed, ill-health can easily develop. Multiple areas can influence this fine balance including digestion, absorption, the location, number and specific species of bacteria, parasitic infection, as well as epithelial integrity and inflammation.
Typical symptoms consist of diarrhoea, constipation, bloating, bad breath, abdominal pain, anemia, food sensitivities and osteoporosis. However, other conditions not typically recognized, but associated with gastrointestinal health, include chronic fatigue, depression, autism, atopy, arthritis and autoimmune disorders.
These conditions may result from ‘leaky gut’ and the subsequent exposure to foreign particles which may trigger local and systemic immune and inflammatory mechanisms.
Smart Gut Microbiome Testing
The smart GUT Microbiome test is a unique test that can only be ordered by an accredited Healthcare practitioner.
Genomic technology now has the capacity to view the human micro biome by sequencing specific regions in the bacterial genome.
This allows bacteria to be identified down to species level. Each bacterial species has a unique “fingerprint”. This means that the analysis is similar to a crime scene investigation. If the sequence is detected then that particular bacteria is present in your gut. It uses Metagenomic Analysis to assess the person’s microbiome.
Metagenomic Analysis involves the sequencing of the thousands of bacterial species present in your stool sample. It is possible to investigate microbial communities by sequencing specific regions in the bacterial genome. The number and amount of microbes can vary greatly from person to person.
SmartDNA DNA Testing
The smartDNA genomic wellness test looks at a variety of pathways in the body and looks for gene changes that can affect how those pathways function. This test can be very useful for people experiencing gut issues as it looks at susceptibility to inflammation, issues with detoxification, predisposition to Coeliac disease and lactose intolerance along with many others.
Inflammation has a key role in chronic disease. Your inflammatory response will be evaluated to reduce your risk of various diseases. It also shows how well your body detoxifies environmental toxins to help reduce your toxic burden. Leaky gut syndrome overloads the body with toxins, if your detoxification pathway is compromised this can place a massive burden on the body.
Breathe Tests
Malabsorption of sugars/FODMAPs
- Lactose Breath test for lactose malabsorption (lactase deficiency)
- Fructose* Breath test for fructose malabsorption
- Sorbitol Breath test for sorbitol malabsorption
Comprehensive Digestive Stool Analysis
The Comprehensive Digestive Stool Analysis is an advanced non-invasive diagnostic tool for assessing gastrointestinal function. The test combines a large number of tests that evaluate the function of the gastrointestinal tract hence a comprehensive picture of a patients gut health can be obtained.
The analysis investigates digestion, metabolism, pancreatic function, the balance of beneficial bacteria and the presence of pathological bacteria, yeast and parasites.
PCR Parasite Test
This is a parasite test that can be obtained free from your GP through Medicare, or for a cost through a private lab referral from us.
Pyrrole testing
Pyrroluria is a genetic condition which inhibits certain nutrients including zinc, B6, biotin and also some Omega fats from reaching targets within the body. It occurs when the synthesis and metabolism of hemoglobin (oxygen-carrying molecules in the blood) is dysfunctional, and an excess of a metabolite called hydroxyhemopyrrolin-2- one is produced. This can affect several biochemical pathways and conditions in the body.
Lactic Acid Yeast Wafers
Lactic acid yeast wafers help restore the bacterial flora of the lower bowel. Lactic acid yeast is a modified form of brewer’s yeast that works in your intestines to produce significant amounts of lactic acid. The additional acid stops the growth of harmful bacteria while allowing good gut bacteria to flourish. Using them along probiotic supplements gives outstanding results…
Benefits of lactic acid bacteria
- Treatment of candida
- Prevention of colon cancer
- Lower cholesterol
- Improving immune function and preventing infections
Probiotic & Prebiotic Foods that promote a healthy Gut
Prebiotic Power Foods
A food that is prebiotic contains ingredients, mostly fiber, that gut bacteria feed on, producing fermentation by-products that benefit health. Here are some of the most potent prebiotic foods:
- Almonds
- Asparagus
- Bananas
- Burdock root
- Cereal grains (whole wheat, barley, rye)
- Chicory root
Probiotic Power Foods
Another way to repopulate good bacteria in your gut flora is through use probiotics. Probiotics are foods or supplements that contain beneficial bacteria.
Instead of being cooked or eaten fresh, probiotic-rich foods are prepared by putting them in a slow cooker or a mason jar or otherwise letting the bacteria ferment them naturally. Common bacteria, like lactobacilli, break down the sugars into acids, preserving the food and imparting a salty, tangy flavor.
Fermented foods can provide fiber for our resident gut bacteria as well as a fresh shipment of transient bacteria. The new bacteria enhance the diversity of our gut microbes during their one-way transit and, in ways that scientists are just beginning to unravel, help the resident bugs do their job better. Here are some of the most potent probiotic foods:
Fermented vegetables (kimchi, sauerkraut, carrots, green beans, beets, lacto-fermented pickles, traditional cured Greek olives), Fermented soybeans Cultured dairy products
Probiotic Supplements
Another effective way to improve gut flora is to take a probiotic supplement.
Probiotic supplements are a convenient way to deliver additional beneficial bacteria to the gut because they don’t require any cooking or meal planning.
Restoring Healthy Gut Flora after Antibiotics & Colonoscopy
Some of the ways to resolve this include the following;
Feed and house the good bacteria that remain in your colon and encourage them to multiply through taking prebiotics which are nondigestible food ingredients that promote the growth of beneficial microorganisms in the intestines.
Avoid use of processed sugar and foods that may contain processed sugar.
Processed sugar feeds bacteria including the germs supposed to be destroyed. This makes difficult to destroy the germs. Hence all sorts of processed foods should be avoided. They should be avoided while trying to rebuild healthy gut flora as well. This is the time to eat a perfect diet. Even varieties of fruit with higher sugar content should be limited at this time.
Take a lot of probiotics for efficiency because some of them are destroyed by stomach acids. For example eating lots of fermented vegetables and other fermented foods can deliver live beneficial bacteria into the gut along with nutrition and enzymes.
Get enough gelatin.
A good quality gelatin is very beneficial for the gut lining. It is highly recommended as a digestive aid, as it can sooth and help heal the digestive track
Reduce your levels of stress. Keep calm!